- Main Page
- A1C Test
- Advance Directives
- Anxiety
- Aortic Aneurysm
- Aphrodisiacs
- Apple Cider Vinegar
- Arrhythmia
- Atrial Fibrillation - AFib
- Back Pain
- Blood Cancer
- Blood Tests
- Blood Test Tubes
- Blood Types
- BMI Calculator
- Body Mass Index - BMI
- Bone Density Scan
- Bone Scan
- BPPV
- Bronchitis
- Cancer Terminology
- Carbohydrates
- Cardiac Catheterization
- Cardiovascular Disease
- Caregiver Glossary
- Caregiver Resources - LGBTQ+
- Caregiver Resources - MO
- Caregiver Resources - USA
- Continuous Glucose Monitors
- Cholesterol
- Citalopram
- COPD
- Coronary Artery Disease
- Cough
- CPAP
- CT scan
- Cyclobenzaprine
- Degenerative Disc Disease
- Depression
- Diabetes Information
- Diabetes - Type 1
- Diabetes - Type 2
- Diabetes - Type 3c
- Diabetes Facts
- Diabetes Care
- Diabetes Care Team
- Diabetes & Fruits
- Diabetes - Gestational
- Diabetes - Pre
- Diabetic Terms
- Diabetes & Vegetables
- Diet - Boiled Egg
- Diet - DASH
- Diet - Fat Burning
- Diet - Mediterranean
- Diet - Military
- Disability
- Disability Permits
- Do Not Resuscitate
- Dupixent®
- Echocardiogram
- E-Cigarettes
- Electrocardiogram
- Electromyography
- Emphysema
- Epidural - Lumbar
- Epidural - Transforaminal
- Epsom Salt
- Facet Arthropathy
- Farxiga®
- Flu - Influenza
- Fluoroscopy
- Gabapentin
- GERD
- Glycemic Index
- Gout
- Headaches
- Healing & Energy Work
- Health Facts
- Health Info. Lines
- Heart Attack
- Heart Disease - Other
- Heart Failure
- Heart Imaging Tests
- Herbal Terms
- Herbal Medicine
- Herb & Oils Uses
- Herniated disk
- HIPAA
- Home Remedies
- Humalog®
- Hydrogen Peroxide
- Hyperglycemia
- Hyperkalemia
- Hyperlipidemia
- Hypertension
- Hypoglycemia
- Hypokalemia
- Hypotension
- Important Numbers
- Indomethacin
- Informed Consent
- Inhalers
- Insomnia
- Insulin
- Juice Fasting
- Juice Recipes
- Kidney Cysts
- Kidney Disease
- Lantus®
- Lemon Benefits
- Lime Benefits
- Liver Disease
- Lumbar Retrolisthesis
- Lung Cancer
- Medicaid
- Medical Specialties
- Medicare
- Medicare - Your Rights
- Melatonin
- Men's Health
- Mental Health
- MO HealthNet
- Mounjaro®
- MRI Scan
- Multiple Myeloma
- Myelography
- Naproxen
- Nasal Polyps
- Nuclear Medicine
- Nutrition - Adults
- Nutrition - Adults, Older
- Nutrition - Kids
- Obesity
- Otolaryngologist
- Oxycodone-Acetaminophen
- Pain Management
- Peripheral Artery Disease
- Parking Spaces
- PET/CT Scan
- PET Scan
- Potassium
- Prednisone
- Prescription Drugs
- Prurigo Nodularis
- PVC's
- Quetiapine
- Quit Smoking
- Radiculopathy
- Red Yeast Rice
- Reiki
- Salt & Sodium
- Salt Water Flush
- Sciatica
- Service Animals
- Sleep Apnea
- Sleep Disorders
- Sleep Studies
- SPECT Scan
- Spinal Stenosis
- Statins
- Stents
- Stress Test - Exercise
- Stress Test - Nuclear
- Sugars - Sweeteners
- Support Groups
- Tardive Dyskinesia
- Testosterone
- Trazodone
- Ultrasound
- Vaccines 19 and up
- Vaccines by Age
- Vaccines 0-6 yrs
- Vaccines 7-18 yrs
- Ventricular Fibrillation
- Vertigo
- Vital Records
- Vital Signs
- Vitamin B12
- Vitamin C
- Vitamin D
- Vitamin E
- Vitamin F
- Vitamin K
- Vitamins and Minerals
- Vitamins Recommended
- Water Benefits
- X-Rays
Needed to read PDF's
Blood Cancer
Blood cancer endangers an essential life force: your blood cells. These cells give you energy, help you fight infection and keep you from bleeding too much. When faulty DNA causes your blood cells to become cancerous, the cancer puts all these important functions at risk. Fortunately, there are many effective and safe ways to treat blood cancer.
What Is Blood Cancer?
Blood cancer affects how your body produces blood cells and how well those cells work. Most blood cancers start in your bone marrow. This is the soft, sponge-like material in the center of your bones. Your bone marrow makes stem cells that mature and become one of the following:
- Red blood cells, which carry oxygen throughout your body
- White blood cells, which fight infection
- Platelets, which control bleeding
Blood cancer happens when something disrupts how your body makes blood cells. The cancer cells can’t do the jobs normal blood cells do. Instead, the abnormal blood cells multiply unchecked and overwhelm the normal ones.
Like any type of cancer, blood cancer is a serious diagnosis. But the good news is that more and more people are surviving blood cancer.
Types of blood cancers
There are three main blood cancer types, each with several subtypes:
- Leukemia is the most common blood cancer in the U.S. and the most common form of childhood cancer. Leukemia cells start in your bone marrow and can spill out into your blood. They’re usually immature white blood cells.
- Lymphoma is cancer of your lymphatic system. Lymphoma cells start in white blood cells called lymphocytes. Lymphoma cells can form tumors in places like your lymph nodes. The most common subtypes are Hodgkin and non-Hodgkin lymphoma.
- Myeloma starts in your bone marrow and affects white blood cells called plasma cells. Multiple myeloma is the most common subtype.
Rarer forms of blood cancer include:
- Myeloproliferative neoplasms (MPN). In this cancer, your bone marrow makes too many white blood cells, red blood cells or platelets.
- Myelodysplastic syndromes (MDS). With MDS, your bone marrow makes abnormal blood cells. Sometimes, the blood cells are abnormal because they don’t develop fully. Immature cells are called blasts.
Symptoms and Causes
Symptoms of blood cancer
Blood cancer symptoms vary based on the type. The most common symptoms to look out for include:
- Fatigue
- Shortness of breath
- Swollen lymph nodes
- Frequent infections
Other symptoms include:
- Bone pain
- Drenching night sweats
- Enlarged liver or spleen
- Joint pain
- Persistent fever
- Unexplained weight loss
- Unusual bruising or bleeding (warning signs include tiny red skin spots or purplish skin patches)
These symptoms can happen with noncancerous conditions, too. Having one or more of them doesn’t mean you have cancer. But you should contact a healthcare provider if symptoms last more than a few weeks.
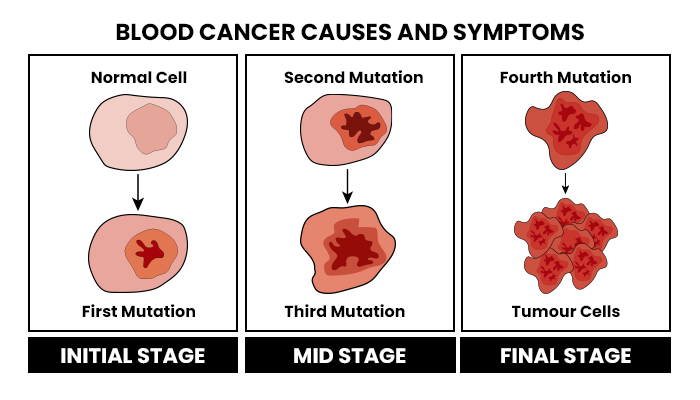
Blood cancer causes
Blood cancer starts when blood cell DNA changes or mutates. Your DNA tells cells what to do. It tells blood cells when to grow, when to divide or multiply, and when to die.
When blood cell DNA gives faulty instructions, your body develops abnormal blood cells. These cells grow and multiply faster than normal. When that happens, normal blood cells become lost in a mass of abnormal cells that crowd out your normal ones.
Eventually, your bone marrow produces fewer normal cells. That means there aren’t enough normal blood cells doing their essential tasks.
Risk factors
Certain factors may play a role in increasing your blood cancer risk, including:
- Age. Your risk increases as you get older.
- Sex. Blood cancers are more common in males.
- Smoking. A smoking history or exposure to secondhand smoke may increase your risk.
- Exposure to toxic chemicals. Long-term exposure to benzene and formaldehyde can increase your risk. You’re more likely to encounter them if you work in an industry like manufacturing.
- Previous cancer treatment. Previous chemotherapy or radiation therapy may increase your risk of developing blood cancer.
- Biological family history. Some types of blood cancers may run in families. But most people who receive a diagnosis don’t have a family member with blood cancer.
- Certain conditions. Several autoimmune diseases, conditions that cause long-term inflammation and some genetic disorders are associated with increased blood cancer risk.
How to lower your risk
Blood cancers aren’t avoidable. Even someone with a clean bill of health can develop blood cancer. But you can lower your risk by steering clear of certain risk factors, like smoking.
Diagnosis and Tests
How doctors diagnose this condition
A healthcare provider may begin by asking about your symptoms and medical history. They’ll also do a complete physical exam. You may need several kinds of tests depending on the cancer type your provider suspects you may have.
Tests include:
- Blood tests for cancer. Tests include complete blood counts (CBC) to check for high or low blood cell levels. You may need a blood chemistry test to check for proteins in your blood that may be signs of blood cancer.
- Imaging tests. Imaging tests can help your provider detect signs of cancer in specific parts of your body. Types include CT scans, MRIs and PET scans.
- Bone marrow biopsy. Your provider may remove a sample of your bone marrow. They’ll analyze how many normal versus abnormal blood cells you have. They may also test your bone marrow sample for changes in your DNA that may drive cancer growth.
Management and Treatment
How are blood cancers treated?
Common treatments for blood cancer include:
- Chemotherapy. Chemotherapy is a primary blood cancer treatment. It kills cancer cells to either slow down the disease’s progress or eliminate the cancer. Healthcare providers use different chemotherapy drug types for different blood cancers.
- Radiation therapy. This treatment uses radiation to damage the DNA in abnormal cells so they can’t make copies. Providers may use radiation to ease symptoms (palliative care). They often combine radiation therapy with other treatments.
- Immunotherapy. This treatment makes your immune system better at fighting cancer. Some of the most commonly used immunotherapies for blood cancer are monoclonal antibodies and CAR T-cell therapy.
- Targeted therapy. These treatments target cancer cell weaknesses that relate to abnormal genetic mutations.
- Autologous stem cell transplant. Providers can collect bone marrow stem cells from your body before giving you high doses of chemotherapy. Once chemotherapy kills the cancer cells, they’ll give your healthy stem cells back to you. They’ll develop into healthy blood cells.
- Allogeneic stem cell transplant. Sometimes, damaged bone marrow needs to be replaced with healthy bone marrow. Providers identify a suitable bone marrow donor and use the donor’s cells to replace your damaged ones.
When should I see my healthcare provider?
Your healthcare provider will let you know what signs or symptoms to look out for after treatment. Every cancer treatment can cause side effects, including potentially serious ones. Your provider will explain how to manage some side effects at home. And they’ll let you know when you should be scheduling an appointment or seeking emergency care.
Prognosis
Is blood cancer curable?
Yes. Often, the goal of blood cancer treatment is curing the condition. This means the cancer is gone, and it never comes back. When a cure isn’t possible, there are a growing number of treatments that may put some blood cancers into remission. Remission means the treatment has decreased cancer to the point that it’s undetectable.
What are the survival rates for blood cancer?
Survival rates vary based on the type of blood cancer. But many people can expect to survive as long as someone without a blood cancer diagnosis. The five-year relative survival rates for blood cancers diagnosed in the U.S. are provided in the table below.
| Blood Cancer Type | Five-Year Relative Survival Rate |
| Leukemia | 67% |
| Hodgkin Lymphoma | 88.9% |
| Non-Hodgkin lymphoma | 74.3% |
| Myeloma | 61.1% |
*Based on data taken from the National Cancer Institute. Surveillance, Epidemiology, and End Results Program from 2014 to 2020.
Remember, though, that no one can predict your life expectancy. For example, certain blood cancer subtypes are more fatal than others. Also, survival rates don’t factor in new treatments that are helping people live longer. After all, the lymphoma survival rate has doubled over the past 40 years. And the five-year survival rate for leukemia has quadrupled over the past 40 years. More and more people are surviving blood cancer.
Is there anything I can do to feel better?
Blood cancer and blood cancer treatment can take a toll on your overall health.
Here are some suggestions that may help:
- Eat nutritious, balanced meals. Blood cancer and its treatment may dampen your appetite. If you’re having trouble eating, ask to speak with a dietitian. They’ll suggest ways to get the nutrition you need to stay strong.
- Stay active. It’s important to get exercise, but ask your healthcare provider what a safe level of activity is.
- Make rest a priority. Pay attention to your body and rest when you need to rest — not just when you feel like you can.
- Protect yourself from infection. Ask your healthcare provider for ways to keep from getting sick.
- Attend to your emotional health. Talking to a therapist or joining a support group can help you during this time. It can help you cope with life after cancer.
One Final Note..
Thanks to new treatments, more people than ever are living with blood cancer. And more people who’ve been diagnosed are in remission. This is great news. But blood cancer is still a serious illness, and learning you have a form of blood cancer is serious business. This is why it’s important to take advantage of every available resource. Understand every available treatment option. Have your provider explain how your diagnosis and treatment can impact your future.
Find me on Social Media
 |
Don't forget to bookmark me to see updates.. Copyright © 2000 - 2025 - K. Kerr Most recent revision May 08, 2026 01:00:38 AM
|











