- Main Page
- A1C Test
- Advance Directives
- Anxiety
- Aortic Aneurysm
- Aphrodisiacs
- Apple Cider Vinegar
- Arrhythmia
- Atrial Fibrillation - AFib
- Back Pain
- Blood Cancer
- Blood Tests
- Blood Test Tubes
- Blood Types
- BMI Calculator
- Body Mass Index - BMI
- Bone Density Scan
- Bone Scan
- BPPV
- Bronchitis
- Cancer Terminology
- Carbohydrates
- Cardiac Catheterization
- Cardiovascular Disease
- Caregiver Glossary
- Caregiver Resources - LGBTQ+
- Caregiver Resources - MO
- Caregiver Resources - USA
- Continuous Glucose Monitors
- Cholesterol
- Citalopram
- COPD
- Coronary Artery Disease
- Cough
- CPAP
- CT scan
- Cyclobenzaprine
- Degenerative Disc Disease
- Depression
- Diabetes Information
- Diabetes - Type 1
- Diabetes - Type 2
- Diabetes - Type 3c
- Diabetes Facts
- Diabetes Care
- Diabetes Care Team
- Diabetes & Fruits
- Diabetes - Gestational
- Diabetes - Pre
- Diabetic Terms
- Diabetes & Vegetables
- Diet - Boiled Egg
- Diet - DASH
- Diet - Fat Burning
- Diet - Mediterranean
- Diet - Military
- Disability
- Disability Permits
- Do Not Resuscitate
- Dupixent®
- Echocardiogram
- E-Cigarettes
- Electrocardiogram
- Electromyography
- Emphysema
- Epidural - Lumbar
- Epidural - Transforaminal
- Epsom Salt
- Facet Arthropathy
- Farxiga®
- Flu - Influenza
- Fluoroscopy
- Gabapentin
- GERD
- Glycemic Index
- Gout
- Headaches
- Healing & Energy Work
- Health Facts
- Health Info. Lines
- Heart Attack
- Heart Disease - Other
- Heart Failure
- Heart Imaging Tests
- Herbal Terms
- Herbal Medicine
- Herb & Oils Uses
- Herniated disk
- HIPAA
- Home Remedies
- Humalog®
- Hydrogen Peroxide
- Hyperglycemia
- Hyperkalemia
- Hyperlipidemia
- Hypertension
- Hypoglycemia
- Hypokalemia
- Hypotension
- Important Numbers
- Indomethacin
- Informed Consent
- Inhalers
- Insomnia
- Insulin
- Juice Fasting
- Juice Recipes
- Kidney Cysts
- Kidney Disease
- Lantus®
- Lemon Benefits
- Lime Benefits
- Liver Disease
- Lumbar Retrolisthesis
- Lung Cancer
- Medicaid
- Medical Specialties
- Medicare
- Medicare - Your Rights
- Melatonin
- Men's Health
- Mental Health
- MO HealthNet
- Mounjaro®
- MRI Scan
- Multiple Myeloma
- Myelography
- Naproxen
- Nasal Polyps
- Nuclear Medicine
- Nutrition - Adults
- Nutrition - Adults, Older
- Nutrition - Kids
- Obesity
- Otolaryngologist
- Oxycodone-Acetaminophen
- Pain Management
- Peripheral Artery Disease
- Parking Spaces
- PET/CT Scan
- PET Scan
- Potassium
- Prednisone
- Prescription Drugs
- Prurigo Nodularis
- PVC's
- Quetiapine
- Quit Smoking
- Radiculopathy
- Red Yeast Rice
- Reiki
- Salt & Sodium
- Salt Water Flush
- Sciatica
- Service Animals
- Sleep Apnea
- Sleep Disorders
- Sleep Studies
- SPECT Scan
- Spinal Stenosis
- Statins
- Stents
- Stress Test - Exercise
- Stress Test - Nuclear
- Sugars - Sweeteners
- Support Groups
- Tardive Dyskinesia
- Testosterone
- Trazodone
- Ultrasound
- Vaccines 19 and up
- Vaccines by Age
- Vaccines 0-6 yrs
- Vaccines 7-18 yrs
- Ventricular Fibrillation
- Vertigo
- Vital Records
- Vital Signs
- Vitamin B12
- Vitamin C
- Vitamin D
- Vitamin E
- Vitamin F
- Vitamin K
- Vitamins and Minerals
- Vitamins Recommended
- Water Benefits
- X-Rays
Needed to read PDF's
Multiple Myeloma
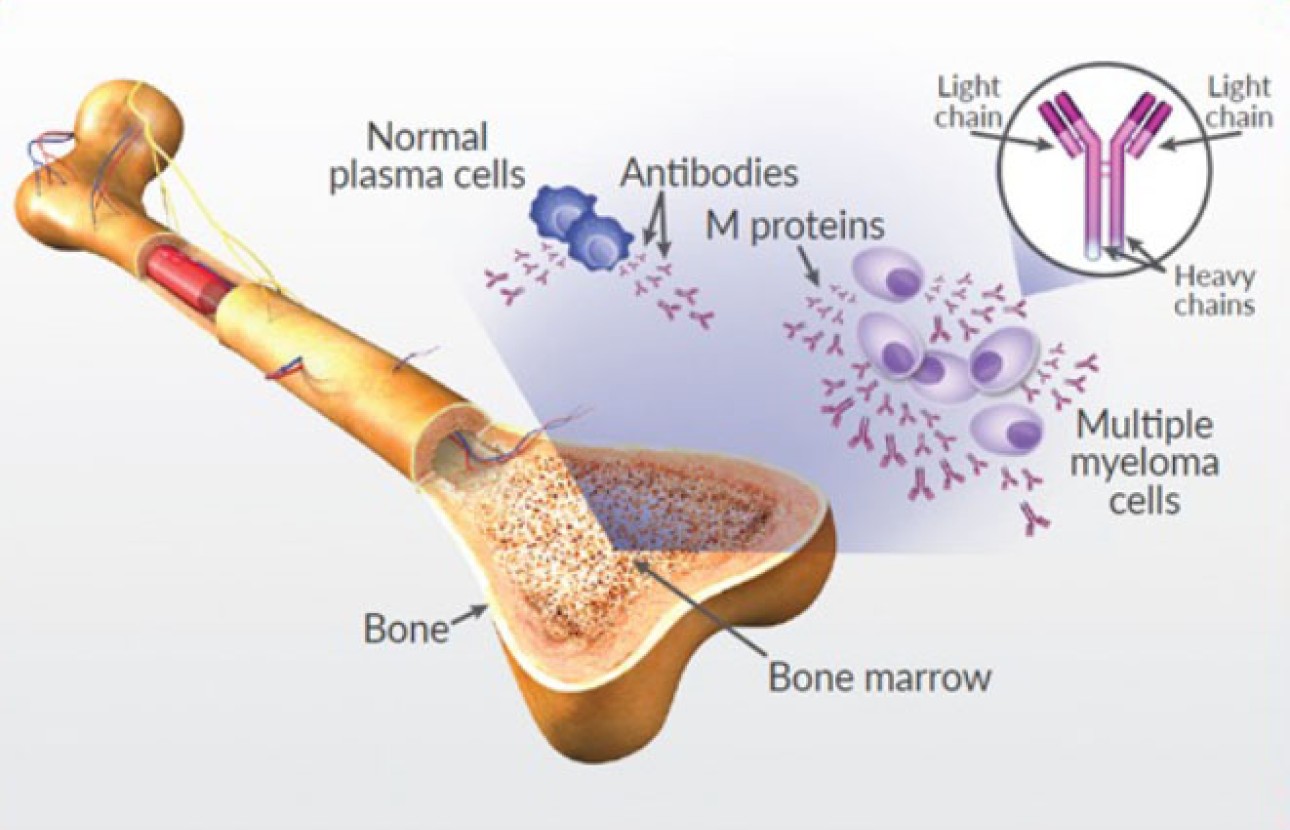
Multiple myeloma happens when healthy plasma cells become abnormal cells that multiply and produce abnormal proteins. This can cause medical issues that can affect your bones, kidneys and blood cells. Healthcare providers can’t cure multiple myeloma, but they can treat related conditions and symptoms and slow its progress.
What Is Multiple Myeloma?
Multiple myeloma is a rare blood cancer that affects your plasma cells. Plasma cells are a type of white blood cell. They make antibodies to fight infection. But with multiple myeloma, plasma cells develop errors and build up in your bone marrow. Bone marrow is the tissue inside bones that makes blood cells. The abnormal plasma cells make abnormal proteins called M proteins.
The cancerous plasma cells can crowd out your normal bone marrow cells. This can prevent your bone marrow from producing healthy red blood cells. This leads to a condition called anemia. The abnormal plasma cells can also damage your bones and kidneys.
Healthcare providers can’t cure multiple myeloma. But they can treat symptoms and related conditions that it can cause. Often, they can slow its progress, so you can live longer.
Symptoms and Causes
Symptoms of multiple myeloma
Bone pain (usually in your back, head, chest, pelvis or upper leg) is often the first symptom people notice. Other symptoms include:
- Fatigue and weakness (signs of anemia, or low red blood cells)
- Getting sick easily (signs of low white blood cells)
- Numbness or tingling in your arms or legs
- Unexplained weight loss
- Nausea and vomiting
Multiple myeloma causes
Medical experts aren’t sure what causes multiple myeloma. But they do know that it happens when there’s a change (gene mutation) in your plasma cells. The mutations cause plasma cells to divide uncontrollably. These aren’t mutations you’re born with. Instead, they happen over your lifetime.
Experts are researching links between specific types of mutations and multiple myeloma. The type of mutation helps providers know how aggressive the disease is. It provides clues about how it will respond to treatment.
Risk factors
Risk factors include:
- Sex: Multiple myeloma affects more males than females.
- Race: It affects twice as many people who are Black as it does people of other races.
- Age: Most people with multiple myeloma are diagnosed between 40 and 70. The median age of diagnosis is 69. A median is a midpoint. Half of the people are younger than 69, and half are older. But generally, it affects older adults.
- Having a family member with multiple myeloma: Rarely, more than one family member has multiple myeloma. But experts don’t know why there’s a link. This condition isn’t hereditary.
- Environmental factors: There may be connections between multiple myeloma and exposure to pesticides, fertilizer or Agent Orange.
- Obesity: Having obesity is a known risk factor for the development of multiple myeloma.
Complications of this condition
Multiple myeloma can lead to other medical issues, like:
- Abnormal proteins damaging your organs (amyloidosis)
- Abnormal proteins damaging your blood vessels (cryoglobulinemia)
- Bacterial infections, particularly pneumonia
- Broken bones
- High levels of calcium in your blood (hypercalcemia)
- Nerve damage (peripheral neuropathy)
Some complications require emergency medical care, including:
- Blood that’s too thick (hyperviscosity syndrome)
- Bones in your spine pressing against your spinal cord (myelopathy)
- Kidney failure
Your healthcare provider will work with you to manage or prevent these complications.
Diagnosis and Tests
How doctors diagnose this condition
Several tests help doctors confirm a multiple myeloma diagnosis. Tests include:
- Blood tests: Providers check for low blood cell counts and enzymes that signal problems with an organ. They’ll also check for abnormal antibodies (like M proteins) and signs of tumors.
- Urine (pee) tests: Your provider may look for high levels of protein in a urine sample that may be a sign of multiple myeloma.
- Imaging tests: X-rays and CT scans can show bone damage related to multiple myeloma. MRIs and PET scans can also reveal myeloma tumors. These are single groups of abnormal plasma cells.
- Biopsy: A bone marrow biopsy tests tissue from your bone marrow for abnormal plasma cells. Or you may need a bone marrow aspiration, which tests the fluid part of bone marrow.
- Genetic testing: Your provider may do a DNA test on the biopsy sample. This test finds gene changes that drive cancer growth.
Precursors to multiple myeloma
Sometimes, people with multiple myeloma don’t have symptoms. Your provider may not suspect anything until blood tests show signs of conditions that may become multiple myeloma.
For example, a biopsy may show abnormal plasma cells, which could mean you have either MGUS or smoldering multiple myeloma. These are early, precancerous forms of multiple myeloma.
Most people with these conditions don’t develop multiple myeloma. Still, your healthcare provider will monitor you closely in case they progress.
Multiple myeloma stages
Cancer staging lays the foundation for treatment. Healthcare providers use the Revised International Staging System (R-ISS) to stage multiple myeloma. It’s based mostly on how many cancer-related enzymes or M proteins are in your blood. Healthcare providers also consider if you have gene abnormalities.
The scale goes from I (growing slowly) to III (growing fast).
Management and Treatment
How is multiple myeloma treated?
Treatment may involve several cancer therapies, with or without a stem cell transplant. A stem cell transplant may slow cancer spread drastically. But not everyone is a candidate.
Treatments include:
- Stem cell transplant: Stem cells are specialized cells in your bone marrow or blood that can help produce healthy new plasma cells. This treatment replaces damaged or unhealthy stem cells with healthy stem cells from your own body.
- Chemotherapy: Chemotherapy drugs reduce the number of abnormal plasma cells. If you get a stem cell transplant, you’ll need chemotherapy first.
- Targeted therapy: This treatment “targets” weaknesses in the plasma cells so they die. People with multiple myeloma are living longer than ever because of new targeted therapies.
- Immunotherapy: This treatment helps your immune system develop more cancer-fighting cells. CAR T-cell therapy is a specific type that has delivered excellent results during clinical trials to test new treatments.
- Steroids: High doses of steroids can kill cancer cells and reduce inflammation.
- Radiation therapy: Radiation can reduce bone tumors causing symptoms.
Other treatments you may need include:
- Medicine for bone pain
- Medicine to prevent bone loss
- Vaccines to prevent infections or antibiotics to treat them
Combination multiple myeloma therapies
Multiple myeloma treatment often involves taking a combination of cancer medications. You may take different types of high-dose chemotherapy drugs. A common combination treatment is called Daratumumab-VRd. It involves taking:
- Daratumumab (monoclonal antibody)
- Bortezomib (targeted therapy drug)
- Lenalidomide (immunotherapy drug)
- Dexamethasone (steroid)
When should I see my healthcare provider?
Both multiple myeloma and treatments to fight it can cause unpleasant symptoms. Some are manageable. For others, you should see your healthcare provider. Ask your provider what symptoms or side effects to expect. Make sure you know when to contact them for an appointment and when to seek emergency care.
Outlook / Prognosis
What can I expect if I have this condition?
There’s no cure for multiple myeloma. But your healthcare provider can help you manage it with treatment. Everyone’s prognosis is different. The overall five-year survival rate is 62%. This means 62 out of 100 people are alive five years after their diagnosis. But the survival rate is higher (80%) when it’s diagnosed in the early stages.
Some people live 10 years or more with multiple myeloma. Much depends on how advanced the cancer is and whether it’s considered high risk.
Your provider will consider these factors as they design your treatment.
Is there anything I can do to feel better?
If you’re living with this condition, it’s important to take things one step at a time. It can be challenging to predict how this condition will affect your body. You can’t always know how you’ll respond to treatment. This is why your healthcare provider will monitor you closely.
Follow their treatment plan. And in the meantime, take care of your body and mind. Getting enough rest and the right nutrition still matters. So does being active — at safe levels. Reach out to a therapist and support groups for emotional support as you work through this diagnosis.
One Final Note..
Multiple myeloma treatments are helping people live longer than ever, with improved quality of life. Still, living with cancer isn’t easy. Treatment and tests will always be part of your life. But know that many others are in the same position. And they’re dealing with this condition in ways that allow them to live fully each day. Reach out to others living with cancer for support. Ask your healthcare provider for resources as you learn what living with multiple myeloma means for you.
Find me on Social Media
 |
Don't forget to bookmark me to see updates.. Copyright © 2000 - 2025 - K. Kerr Most recent revision May 08, 2026 01:01:02 AM
|











